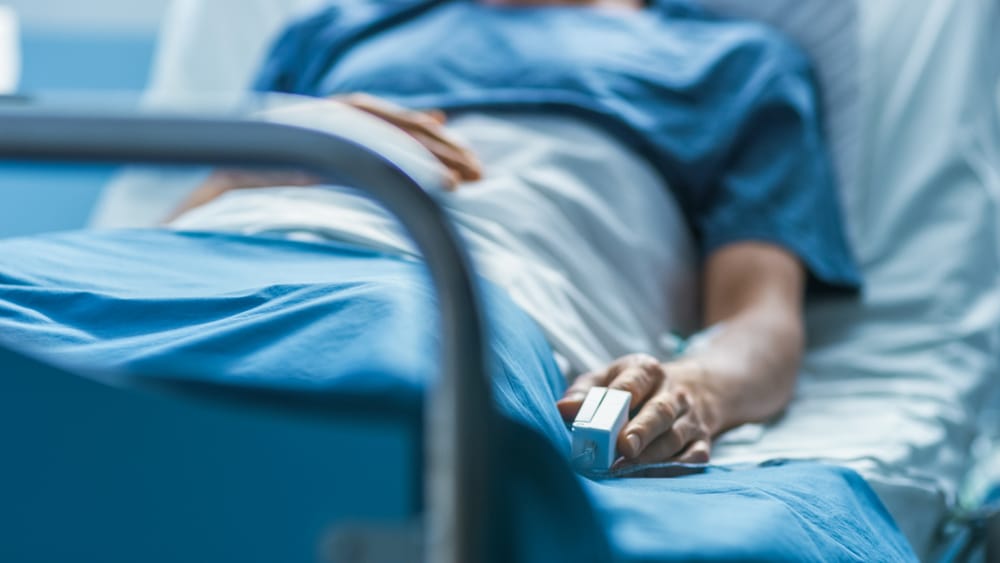
Hospitals are more full than they’ve been throughout the Covid-19 pandemic, according to a CNN analysis of data from the US Department of Health and Human Services. But as respiratory virus season surges across the US, it’s much more than Covid that’s filling beds this year.
More than 80% of hospital beds are in use nationwide, jumping 8 percentage points in the past two weeks. Hospitals have been required to report capacity information since mid-2020 as part of a federal effort to track the effects of the Covid-19 pandemic.
Hospitals have been more than 70% full for the vast majority of that time. But they’ve been 80% full at only one other point: in January, during the height of the Omicron surge in the US. Back in January, about a quarter of hospital beds were in use for Covid-19 patients. But now, only about 6% of beds are in use for Covid-19 patients, according to the HHS data.
The broader respiratory virus season is in full swing across the US. All but six states are experiencing “high” or “very high” respiratory virus as seasonal flu activity remains “high and continues to increase,” according to the US Centers for Disease Control and Prevention.
The number of people admitted to the hospital for flu during the week of Thanksgiving was nearly double the number of admissions during the week before. And the latest surveillance data probably does not reflect the full effects of holiday gatherings, as it captures only through November 26, two days past Thanksgiving.
Nancy Foster, vice president for quality and patient safety with the American Hospital Association, says that an influx of flu patients is a key reason why hospitals are filling up.
“The rates are higher because we are seeing many patients with the flu season in many parts of the country and that has brought a lot of older adults and some young children into the hospitals,” she said in a statement to CNN. “Additionally, RSV is filling many pediatric beds and cribs.” On top of that are challenges brought on by workforce shortages and a backlog of patients who delayed care over the past few years.
“Patients whose care may have been delayed earlier in the year for either because of Covid spikes or because of critical staff or supplies are now being treated,” Foster said. “Workforce shortages have not only made it more challenging for hospitals but also have diminished the number of patients who can be cared for in nursing homes and other post-acute care settings. Thus, patients are spending more time in hospitals, awaiting discharge to the next level of care and limiting our ability to make a bed available to a patient who truly needs to be hospitalized.” (SOURCE)